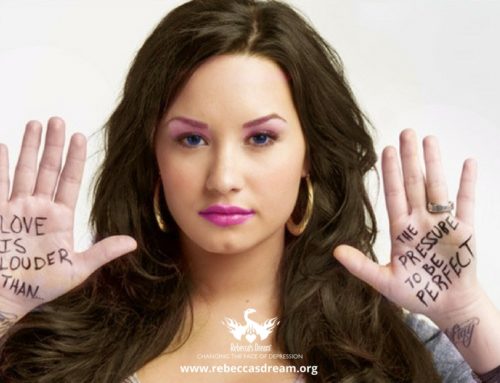Compassionate understanding helps remove stigma.
Since the days of ancient Greece, when Hippocrates attempted to uncover more information regarding “melancholia” or “black bile” as it was then referred to, doctors have been striving to understand and treat depression or major depressive disorder as it is now termed by many healthcare professionals.
Although the tide is turning with regard to depression being recognised and accepted as a genuine mental illness, there is still misunderstanding and at times, intolerance and a lack of compassion with respect to this condition. There is nothing “shameful” in having a mental illness, but unfortunately there is still stigma attached to this in contrast to the more understanding and caring attitudes generally engendered by physical illness. Unfortunately, people suffering from depression can still be judged as being somehow ungrateful, weak or indulging in self-pity, purely because their condition is not physically visible and this means that it is often concealed and much needed help is not sought.
Co-author of, “The A-Z Guide to Good Mental Health” and expert on mental wellness, Jeremy Thomas states. “Mental illness is no more about failing or failure than a physical illness. It happens.” He continues. “The first step in fighting depression is recognising it and deciding to seek help. Sometimes getting help can be difficult in itself and you may need to keep trying. You are not alone. Depression is, in the majority of cases, eminently treatable, and the sooner you can begin to access help (social and professional) the shorter this debilitating illness is likely to last.”
While most people feel subdued and emotionally “flat” from time to time, clinical depression makes life very difficult indeed. Other categories of depression include mild depression, bi-polar (formerly known as manic depression), postnatal depression, prenatal depression, dysthymia and seasonal affective disorder (SAD). Similar to an anxiety disorder or an addiction such as alcoholism, someone is much more likely to suffer from depression if a member of their family has had a history of the illness. The National Health Service (NHS) states. “Doctors describe depression by how serious it is: Mild depression – has some impact on your daily life. Moderate depression – has a significant impact on your daily life. Severe depression – makes it almost impossible to get through daily life; a few people with severe depression may have psychotic symptoms.”
Although medication is usually suggested by GPs, mindfulness is also proving to help many sufferers ease the symptoms of depression and reduce the likelihood of a full-blown relapse. Since the early 2010s, Mindfulness-Based Cognitive Therapy (MBCT) has received much media coverage, primarily because of the well researched data by Zindel Siegal and Professor Mark Williams. UK MBCT explains. “Mindfulness takes a different approach. It helps develop our willingness to experience emotions, our capacity to be open to even painful emotions. It helps give us the courage to allow distressing mood, thoughts and sensations to come and go, without battling with them.” The MBCT research continues. “We discover that difficult and unwanted thoughts and feelings can be held in awareness, and seen from an altogether different perspective – a perspective that brings with it a sense of compassion to the suffering we are experiencing.”
Generally speaking, it is suggested by most medical doctors and counsellors to enquire about depression if one has been feeling hopeless and very low for more than four weeks. It is always best to seek professional advice because a person may misdiagnose themselves as being depressed when they are actually grieving a loss. Grief is a natural human response to a loss (although suppressed grief can be very serious – read my HuffPost UK blog on ‘healing from trauma and frozen grief’), whereas depression is a mental illness. It is crucial to seek help if this illness is suspected and even more important not to isolate. Depression thrives on isolation.
To learn more about bipolar disorder, depression, anxiety or suicide prevention please visit our website.